I worked abroad as an engineer for many years in Australia, America and Asia, so we spent a lot of time apart. But we all lived in Singapore for eight years before settling in Shropshire.
Linda cared deeply about young people. She set up lots of youth groups and always made everyone feel welcome. She was a devout Christian and had an incredible faith, and also worked as a nurse for many years.
Ruth: Mum’s family was her life. She managed to make anywhere a home, wherever we lived across the world. All my friends used to come to the house to talk to Mum; no subject was off limits.
When Mum died, we were getting calls from men and women in their 60s who she had supported through her youth work – some living as far away as Uganda.
“We had to find everything ourselves” – Kip
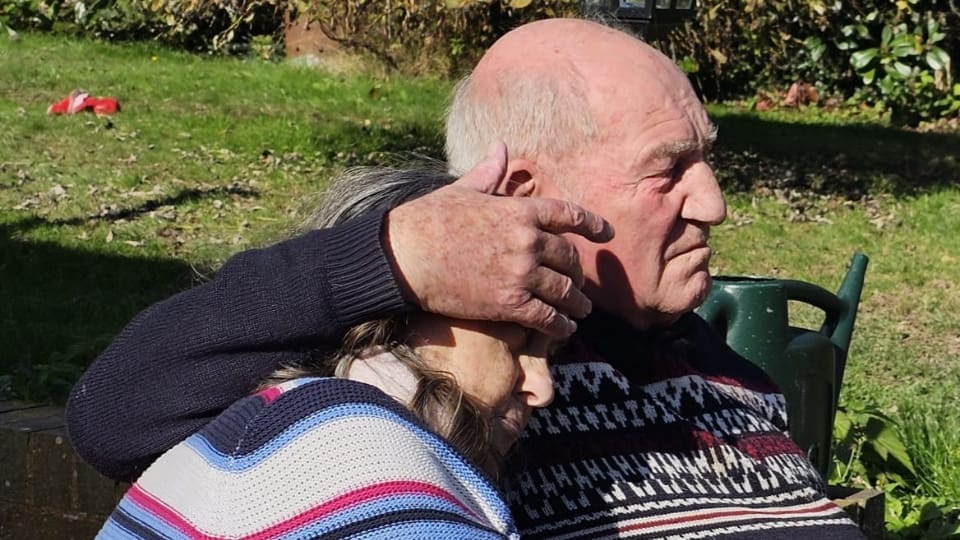
Kip and Linda
Ruth: We started to notice changes in Mum’s behaviour during the Covid pandemic. In January 2021, my sister and her children came to visit us in the garden on Mum’s 76th birthday. Mum became very stressed after they left and couldn’t understand why they weren’t allowed to come into the house. A couple of hours later, Mum had no memory of them coming and was upset that they hadn’t visited on her birthday.
It started to click that Mum might have dementia, but it took us eight months to get a diagnosis. At this point, we were told that Mum would likely live for around four to five years – but the only support we were offered was a booklet.
Kip: We were told by the GP that Linda had dementia and that there was nothing they could do for her. I wish that we had been told about the support that could have been available to us, but we had to find everything ourselves. It was hard.
Ruth: As Mum’s dementia progressed, every day was a challenge. She would put a packet of raw mince on the stove in plastic wrapping. She started to experience episodes of psychosis and would phone me to say there was a strange man in the house. It was Dad, but she didn’t recognise him.
Mum also got it into her head that the tablets she was taking for psychosis were making her unwell. She really didn’t like taking them, and we would find them in her shoes, plant pots and cupboards. We’re still finding tablets in hidden places to this day.
Dad weathered the storm alone for a long time. But we made Mum a promise that we would keep her at home, so I moved in to help. Caring for her had become a two-man job.
“I phoned the Dementia UK Helpline in desperation” – Ruth

Linda and Ruth
Kip: As Linda’s dementia progressed, we tried to reach out for help, but we kept running into brick walls. I wish someone had just told us about end of life care.
Ruth: Mum went downhill quickly in the final two weeks of her life. She was having bouts of terror. We would have to lie with her on her bed until she cried herself to sleep.
In desperation, I phoned Dementia UK’s Helpline. They recognised that we were an urgent case and referred us to an amazing dementia specialist Admiral Nurse called Kerry, who specialised in supporting families with issues relating to frailty and physical health.
Kerry stepped in quickly, and her support meant everything to us. For the first time in four years, we didn’t feel alone.
When I told Kerry that Mum wouldn’t take her medication and that she had started pulling food out of her mouth, she explained that Mum was on an end of life path. I thought, “What on earth is that?” I’d never heard that term before despite having told the GP everything that I’d told Kerry.
Kerry said that Mum appeared more well than she actually was as she was overweight and mobile. She also said that as Mum had been a nurse, she would put on a show in front of other healthcare professionals.
When I went back to the GP to explain what Kerry had said, I met with a lot of resistance. I made another phone call to Kerry, and she wrote me a script of everything I needed to say to the GP. This included asking for a liquid form of any necessary medication, anti-anxiety medication for Mum’s terror, an end of life medical bag in the house, and a referral to the local hospice to set up a respite care path as Mum would be dying at home.
“I listened to Mum scream in pain all night” – Ruth
The GP started the process, and I picked up the liquid meds on Friday. But early on Sunday morning, Dad came in to tell me that there was something seriously wrong with Mum. She was sitting on the edge of the bed, and she wouldn’t speak or move. I phoned 111 and it took 18 hours to get a doctor out. Mum sat on the edge of the bed the whole time and screamed if we tried to lay her down.
When the doctor arrived, he gave Mum an injection of morphine and said he was fairly certain that she’d had a stroke. He said mum should be fine through the night, but she wasn’t. I called back every hour and a half before finally, another doctor came out and told us that we should have been given the local end of life service number, as they get a doctor to you within an hour. We had four doctors visit through the night.
At 8am I phoned the GP, having listened to Mum scream in pain all night, but had still had no response by 10am. When the doctor eventually arrived, she didn’t have any syringes to administer the morphine and said that it was the job of the district nurses, but we had never met them.
Thankfully, the district nurse turned up about an hour later and took control of the situation. She came back with a morphine pump system.
Soon after, Mum had a second stroke and from that point, she was unconscious. She passed away at home six days later. While her last days were incredibly traumatic, we’re grateful that dementia never got to the core of who she was and the love she had for the people in her life. She recognised us right up until the day she died.
I spoke to Kerry just hours before Mum died. We both knew what was about to happen, even without having to say it. Kerry made me feel less alone.
Kip: We believe Linda is in a better place, which helps us process our grief. Years ago, someone gave Linda a cross made from olive wood from the holy land. During the last two days of her life, she wouldn’t let go of it. She died with it in her hand.
“We want to make the process easier for other families” – Kip
Ruth: When Mum was at the end of her life, we didn’t know what help to ask for and without Kerry, we wouldn’t have even known to ask for it. And as it turned out, unfortunately, we asked for it too late.
We found out that we could have turned the bathroom into a wet room to make it easier to keep Mum clean, as she was doubly incontinent. We could have been trained to administer the morphine ourselves. We could have had an inflatable mattress and sliding sheets to make it easier to move Mum. I’m particularly angry that she could have had liquid anti-anxiety medication to stop that awful fear. But we found out about all of these things too late, which shows how badly the system is falling apart.
We asked to have a conversation with the GP as Mum had experienced so much unnecessary pain at the end of her life. All the GP said was, “Opportunities were missed.”
Kip: All we want to do now is make the process better for other families, so they don’t have to experience what we went through. GPs should let families know about what to expect at the end of life and the support that’s available. It could be as simple as a piece of paper given to families with information about what to expect and what help is available. You shouldn’t have to figure it all out yourself.
We’re intelligent people; I’m an engineer, and I’ve started nuclear reactors with fewer problems. We’re also a very tight family, and we got through it together, but not everyone will have a family like ours.
Ruth: When you’re told that your loved one’s life is coming to an end, there are things you can do to prepare. We were completely reliant on other people and totally blind. Death is a hard thing to face and end of life care is very specialist. The more prepared you are, the better you will face it.
“I’ve never met Kerry, but she held my hand” – Ruth
Kip: The support from Kerry felt like we were lost at sea and then a lifeboat came to rescue us.
Ruth: I really want to raise awareness of Admiral Nurses. If we had known about them even two months earlier, we would have benefited so much more from the support. My advice to anyone in a similar situation is to phone Dementia UK and speak to an Admiral Nurse as soon as you can.
Without Kerry giving us guidance, it would have been horrendous. I’ve never met her in person, but she really held my hand. We couldn’t have got through it without her.






